Screening for Liver and Kidney Disease Exposure to hazardous or toxic substances can affect the body in many ways. In general, when chemicals and other hazardous substances are absorbed, they travel through the various body systems and can affect a particular organ or organs, called the “target organ(s).” Fortunately, the body has mechanisms, mainly in the liver and kidneys, to process and eliminate many of these substances. This ability to eliminate toxic substances can reduce the effect(s) on the target organ(s). The elimination of toxic substances is just one of the many functions of the liver and kidneys. For example, the kidneys maintain the blood volume and regulate the mineral content in the bloodstream. The liver converts nutrients into energy, forms proteins and stores carbohydrates. While these organs can be remarkably resilient in the elimination of toxins, their other functions can be damaged in the process. Damage to the kidney and
liver can be acute or chronic. An acute process generally refers
to a relatively short period of time (hours to weeks) between
exposure to the toxin and the onset of symptoms or medical findings.
A chronic process generally refers to a long period of time (years)
between exposure to the toxin and the onset of symptoms or medical
findings. The detection of either an acute or chronic process
or disease can be complex, depending on the type of toxin and
the extent of exposure.
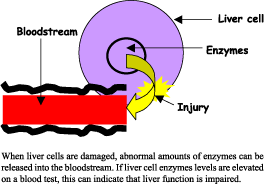
How Do You Detect Liver or Kidney Disease? There are several tests available to detect abnormalities. Blood tests --- commonly referred to as liver and kidney function tests --- are among the most commonly used. In a typical blood chemistry profile, six liver function and two kidney function tests are done. See box. What are Liver Function Tests? What are Kidney Function Tests?
What if These Tests are Elevated? There are many diseases and conditions that can cause an elevation of these tests. Some of the more common causes are hepatitis (inflammation of the liver) from infectious agents such as viruses and substances such as alcohol. Some common causes of kidney damage include diabetes and high blood pressure. Kidney and liver damage may also be work-related. There are certain organic chemicals (such as carbon tetrachloride) that can cause both liver and kidney disease. Certain metals (lead, mercury, cadmium and uranium) are known to cause chronic kidney disease. Since many toxic substances are difficult to detect in the body, a detailed occupational history is essential for determining whether kidney or liver disease is work-related. Liver and kidney function tests, once documented to be elevated,
need to be monitored periodically, depending on the degree of elevation
and the overall medical circumstances. Further tests may be done
to determine more precisely the extent of damage. Besides follow-up
tests, it should be emphasized that if a particular chemical substance,
whether work-related or not, is causing the abnormality in the liver
or a kidney function tests, exposure should be stopped to prevent
further damage to these organs. Workers also need to minimize exposure
to workplace liver and/or kidney toxins if they have kidney or liver
disease of any origin. |